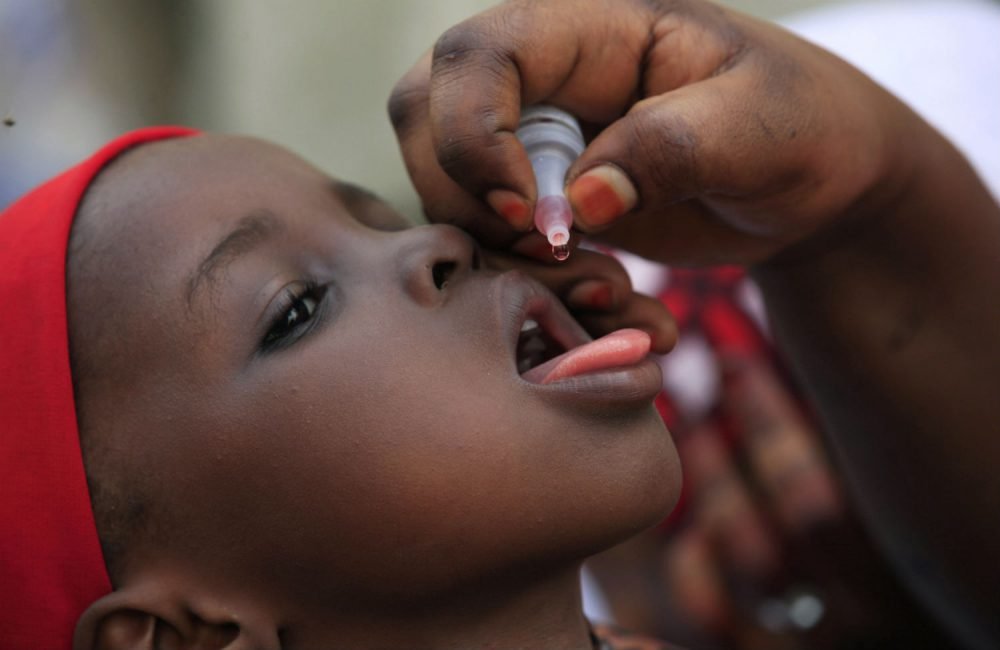
The Sokoto State Primary Health Care Development Agency (SPHCDA) has said old beliefs and sermons against polio vaccines have been a blight on the fight against polio, as hesitancy persists in the state.
In this exclusive interview with PREMIUM TIMES, the State Immunisation Officer (SIO), Bashar Garba, said many who still refuse the vaccines have their beliefs fixed for a long time and are not newly influenced.
Mr Garba expressed concern that the highest rates of refusal are in metropolitan local government areas (LGAs), not in rural LGAs.
According to him, Sokoto North, Sokoto South and Wamakko – all metropolitan LGAs – have taken turns topping the chart, but have collectively retained the top three positions in non-compliance.
He said the state is working with over a dozen local and international partners in the fight against polio resurgence, following the 20 cases of the circulating Vaccine-Derived Poliovirus Type 2 (cVDPV2) recorded last year. The cVDPV2, a strain of poliovirus causing paralysis in under-immunised populations, has caused more polio cases annually than wild poliovirus since 2017, according to the WHO.
Mr Garba also listed the challenges still being faced and the progress made so far on immunisation coverage.
Here is the transcript of our interview with Mr Garba, Sokoto state’s number one man on immunisation. It has been lightly edited for clarity and brevity.
PT: I want you to tell us about the immunisation coverage of Sokoto State. Where are you currently? What are the trends like?
Mr Garba: About immunisation in Sokoto, the coverage follows a two-phase approach. There’s what we call routine immunisation coverage, and there’s what we call supplementary immunisation activities coverage.
Routine immunisation coverage is immunisation that occurs routinely and targets children under 5 years old in the state. It usually happens at the health facility and the outreaches. For Sokoto, based on the previous survey, our coverage is still below 15%.
Looking at the Penta-3 coverage. According to the recent Demographic and Health Survey (DHS), in Sokoto, the Penta-3 and other antigens are around 60%.
For the supplementary Immunisation Activities (SIA), which include polio campaigns and other polio-related campaigns, such as the Measles Rubella campaign, we just concluded during the October round. We’re having almost 97 per cent campaign coverage. Our portfolio that we just concluded last November, we’re having 101 per cent coverage. So these are the campaign’s coverage.
PT: Nigeria was previously declared polio-free, but in the last two years, there have been reports of new polio cases, which have raised concerns. Has your agency investigated the reasons behind the resurgence? What factors led to these cases, and what measures are being put in place to ensure that polio does not re-emerge in Sokoto State?
Mr Garba: With regard to the recent report of the polio cases, it is type two. Type one is the Wild Polio Virus (WPV). That one has been eradicated, and it’s the most dangerous type of polio. But the cases we had are all type two.
Last year, we had over 20 of those cases in Sokoto, though some were directly from the children, and others were detected in the environment through sampling gutters and other areas.
This is a very serious concern. Sokoto State continues to put a lot of effort into ensuring that it stops the transmission of the cVDPV, looking at the danger behind that disease. Last year, with the support of the National Primary Health Care Development Agency (NPHCDA), we implemented five rounds of the polio campaign, although we still have concerns about data quality and performance. Also, the state is doing its best to ensure that it holds people accountable for their actions, especially regarding the quality of their performance.
So, I understand the majority of teams in the states don’t visit all the households. The majority of households will be missing because the team will just be denied access, or the team intentionally doesn’t want to visit those houses.
Also, we observed that many children missed vaccination due to refusal. A lot of people, especially in the metropolitan LGAs of Sokoto South, Sokoto North, and Wamakko, are refusing oral polio vaccines. Most of the reasons have to do with religion; they believe that the polio vaccine is not safe, and some refused it for political reasons. They reject it because of political differences with the current government. And some it’s just poverty. They just prefer to be given rice, beans, and other food commodities rather than any vaccines. These are some of the reasons why we keep having low acceptance from the community. And this is a serious challenge.
The Sokoto state government and the other partners are addressing those issues regularly. So, there are a lot of advocacy, sensitisation meetings, and even compound meetings to ensure people are sensitised to the importance of those vaccines.
PT: You talked about the refusal by some households, and also the fact that some of them are even metropolitan LGAs, not rural areas. What steps is your agency taking to address this refusal and encourage more people to accept the vaccines?
Mr Garba: Whenever we are going to have a campaign, the Sokoto state government organises a lot of serious meetings, especially engaging the elite, because the non-compliance doesn’t come from people who don’t have a Western education. It comes even from people who have a degree.
So there’s elite sensitisation. A lot of people will be invited and sensitised to the importance of taking polio vaccines. Also, there are many non-compliance solution committees composed of well-recognised women and men in the area, who will be engaged and provided with transport so they can go area by area to encourage those who refuse to accept the vaccines. So this involves doctors, businessmen and youth leaders. These are the committees that we named as the Rapid Response Team (RRT), which are going after those who refuse the vaccines. So this is what the state is doing.
Also, there is a lot of mobilisation. There’s what we call a motorised band, a lot of motorcycles with megaphones, and others will be going into town to remind people of the importance of accepting the polio vaccine. The campaign is ongoing. Also, there are many phone-in programmes where the honourable commissioner for health, the executive secretary of the state primary healthcare development agency, and other senior colleagues will be live on television or radio, answering many concerns regarding the polio vaccines and campaign on air.
Also, there are a lot of banner distributions and a lot of radio jingles just to create awareness and tell people that this is very important.
PT: Which Local Government Areas are the most non-compliant with the vaccines?
Mr Garba: So, based on the recent analysis we have, the metropolitan. Number one, the leading non-compliant LGA in the state is Sokoto North, followed by Sokoto South and Wamakko. And things keep changing. When we have a round today, you see Wamakko is leading. Sokoto North is second, South is third. But these are the prominent non-compliant LGAs that we have in the state. Even nationally, because I can remember there was a campaign that we did. Kano and other northern states implemented it as well. Arkilla Ward in Wamakko LGA was the leading ward in terms of rejections and non-compliance during that campaign. So, that shows how Sokoto is facing significant resistance to polio vaccines.
PT: One more thing I want to know. Have you been able to identify certain influential individuals in the community who instigate people to refuse these vaccines?
Mr Garba: No. For now, we don’t have any influential person who is preaching or encouraging people to refuse. But we have influential people who are refusing. Though they are not encouraging others to refuse. But some people are following them, so if they refuse, they too can refuse.
What we observe in Sokoto is that there was a time, a long time ago, when we saw a lot of preaching from Islamic religious leaders against polio specifically. So the audios are still in circulation. Sometimes, you can hear this from social media. If you view some old media (recorded) from the past 10 years or even 20 years, you might think that polio vaccines are not good. So that is the challenge we have. People are still using the preachings that happened a long time ago to stick to refusing the vaccine.
Some will even tell you that, even if he (the preacher) accepts it now, they won’t accept it because they believe he already said the truth and now he’s just changing his mind for money or any other reason. So, that is the challenge that we have. And this refusal is what has continued to make Sokoto a higher burden of the cVDPV2.
PT: I understand you are trying to scale up coverage this year. Can you tell me about the plans you have for immunisation coverage?
Mr Garba: Not only coverage, I think even toward the end of 2025, but there’s also a lot of interventions and a lot of routine immunisation (RI) intensification, to see that our routine immunisation coverage is good.
So, our priority for 2026 – for the Ministry of Health, as well as the primary health care development agency – is to see how we can scale up our routine immunisation coverage and even interrupt the transmission of this polio, cVDPV2.
Our preparation has to do with how we are going to implement a higher level quality polio campaign, a campaign that will be accepted by everyone and a campaign that will ensure each and every eligible child is being vaccinated with important polio vaccines. How can we do that? That is the preparation we are still doing. You have even seen us now having a lot of discussions and meetings.
Number one, we want to do what we call IEV – I, identify the eligible children, and E, enumerate them, and then V, which is going to be vaccinating them. We plan to ensure that each and every eligible child under five is identified in Sokoto state. And those children are being enumerated so that we have a soft and hard copy of their data, so that we’ll have a tracking number to track them when vaccinated. And if they are not vaccinated, we’ll see from the summary that so-so numbers of children with this address have not been vaccinated. This is what we want to do. We are going to commence this on Saturday, 14th of February, and to go on to run for like four to six days.
After that, we’ll ensure that the enumeration is concluded and finalised. On 7th of March, during Ramadan, when a lot of children will be at home. We’ll go there and vaccinate those children.
The second plan is to boost our routine immunisation. We have a target, every quarter or biannually, we’ll do a vaccination with the inactivated polio vaccines (IPV), which is a very strong vaccine, that is an injectable. It’s a very strong vaccine that can prevent all types of polio viruses. We want to use it at least once a year, because it’s a very expensive campaign. It requires a lot of resources.
We currently have a plan supported by the Solina Centre for International Development and Research (SCIDaR) to put our intensification teams across all six LGAs that have borders with Niger Republic. And this one will be carrying routine immunisation vaccines, including the polio, so that each and every child living in those border communities is being protected. And any child that is crossing is going to be vaccinated so that they cannot go out with the virus to Niger or come in with the virus to Nigeria. These are the brief plans I can tell you with regard to the preparation to improve our coverage for immunisation in 2026.
PT: That’s quite a robust plan. I like that you mentioned the partnership with Solina, but I also know that you have many more partnerships with different organisations. Can you talk about some of these partnerships and what those partnerships entail?
Mr Garba: For Sokoto, we have more than 15 partners that support immunisation. I can just take you through some of the major partners, starting from the WHO, UNICEF, CDC, AFNED, Solina, eHealth, and Res4Sahel, which usually have a rich programme, and McKean, Aliko Dangote Foundation, BMGF, Healing Killers, a lot of them.
There are some partners that support the state technically only –they support capacity building of the state’s personnel– and there are some that support financially also, like WHO. They usually support the states in building the capacity of state teams, local government teams, and they support the state with some funding and implementation of some of the immunisation activities. UNICEF, especially during campaigns, supports the state intensively in terms of logistics, team transportation, fueling of generators, storage of vaccines, and also social mobilisation. UNICEF supports the state very well in terms of social mobilisations. UNICEF also has some personnel recruited, volunteer community mobilisers (VCMs) who used to go house to house in the city and mobilise women of childbearing age, or pregnant women and the children just to go to the nearby health facility for Ante-natal care (ANC) or routine immunisation. Also, during polio, they ensure that each and every eligible child in their settlement, when they work, is being reached and vaccinated.
There’s also New Incentives. They are into immunisation, and they support the state in ensuring they reduce the hardship of women who can not afford transportation. So they give them some incentives, monetised incentives. Also, the Médecins Sans Frontières (MSF). Currently, we have an outbreak of diphtheria in the state, and the MSF supports the state with the vaccines as well as the operational costs.
There’s also CHI, there’s Chigari Foundation, Sultan Foundation, we have a lot of them. There’s a lot, I can’t mention all of them,
PT: That’s interesting. I know you’ve done a lot, and you’re still doing a lot. I would like you to talk about some of the improvements or achievements that you have recorded from these campaigns
Mr Garba: There are, there must be. Though we are not there yet, the quality of our campaign has improved. Because previously, the way we did our campaign, it would be very difficult to just come out and point and say there’s a problem. But now, even from the preparation, you can know whether things are going well or not, because of how we digitised our system.
Whatever we are doing now, we use a digital form. Even the documents, the papers, we are using to obtain data from the house-to-house teams, we are using e-tally, where the number of children vaccinated will be entered. And even the geo-coordinate that shows that these teams are going house-to-house.
Unlike before, we collect a paper tally. That paper tally, we have to assign somebody who will be collecting it on a daily basis, and that person will submit it to the state. Previously, it would take like four to five days after the campaign, before we run analysis on that paper and know that there’s a gap. But now, the data team can pull it out and see that you are not doing well immediately. So this is an improvement. Also, even in how we do our micro-plan, there’s a lot of improvement.
There’s a lot of improvement in how we update the master list of settlements. Previously, it was manual, paper-based, but now everything is computerised. If a settlement is inhabited or uninhabited, if the settlement is secure or insecure, if the settlement is hard to reach, you can immediately sort it out from your computer and say, this is the result.
It’s just for us to go physically and validate those submissions. So there’s a lot of improvement. And now, as I mentioned earlier, on a daily basis, we can track the performance. Immediately, you say you have done this, a data person can enter into the computer and say, yes. If you say you are at EOC, and you are at your home sitting down, a data person will pull it with the geocoordinate and tell you, no, you are not at EOC. So there’s a lot of improvement, actually.
PT: That’s great. Finally, I know sometimes, no matter the kind of improvement, you still realise there are certain issues. Are there challenges that you still face, despite all of these improvements?
Mr Garba: Yes, the challenge that we have as a state with regard to these interventions, I can tell you in two ways.
Number one, if you take the supplementary immunisation, which is the polio campaigns, our major challenge has to do with our teams. We have a serious concern with the performance of our team members. The majority of our team members, despite the rigorous process of identifying and selecting them, are not doing well. Most of them are not honest. We need to have a very serious mindset change for people to understand that they need to tell the truth, just to help the community.
In a situation where we follow all the criteria, pass through the traditional leader to nominate the team members, screen them, select the best of those submitted, train them, give them all the required training that they need, and even give them transport. Then they will go to the households, collude with caregivers who refuse vaccination, and finger-mark their finger with the assumption that anybody can just show them that we vaccinate. So you see, this is serious.
The programme and the coordination are doing their best, but our team members are not sincere and are not helping the situation. At the end of the day, the virus will come to the house and affect the children, because the children were not vaccinated. The house and the house marking continue to show acceptance, despite the fact that the children, in reality, didn’t get the two drops. So this is what we have as a serious issue.
Because if you know the concern, it will be easy for you to coordinate to resolve it. If you come and tell me, so-so-so house refused, it will be easier for me at the state level to make a proper plan on how we are going to reach those people and resolve their concerns. This is the issue we have observed for a long period of time in the campaign.
The teams are concealing non-compliance. They are doing finger marking without vaccination, and that means fake finger marking. So this is a serious concern.
Secondly, still with the teams, though we have a tracker that will track how the teams perform, the quality of their activity is a serious concern. What I mean here is that a vaccine needs to be at a cool temperature. From where you pick it up to the point that you’re dropping it. But there’s a lot of compromise. You can visit the vaccination teams, and they will just open the cap of the vaccine throughout the visitation. They will not even close it.
ALSO READ: Immunisation vital to polio eradication in the world, says Rotary International President
They will expose it to the sunlight. And these vaccines are light attenuated. They are sensitive to any light. Once exposed to light, you are just killing it. You are reducing the potency. So that is another technical issue. The majority of them will just open the vaccine. They will not even close it and continue to move. The vaccine is being exposed. Some will put it inside a sachet or nylon and hold it. So these are some of the technical issues that affect the quality of the campaign.
When you come to routine immunisation. In Sokoto, we observe two to three things. Number one, actually, the government is trying their best. Now, there’s a lot of recruitment. More than 1,000 primary health care workers are being recruited. What remains is just for them to commence work, and these are the efforts of the current government. But before that, we have very inadequate routine immunisation service providers. There are not enough. You could go to the health facility, and you would see only one person. He’s the one giving RI; he is the one seeing patients if they are sick. And he’s the one recording the people who visited the health facility for RI or for any other reasons. So you see, the workload is too much.
So to the extent that, maybe today, tomorrow, next tomorrow, I must be in the health facility. But maybe Thursday, Friday, I need to go to the nearby settlement, so that I can implement the outreaches. Because of the workload, you’ll find out at the end of the day that he may not be able to go out. And those people who are waiting for him to come because he’s very far away from them, they can’t come, and they will miss the opportunity.
And when a survey comes, they may pick that settlement where he stayed for a long period of time without visiting. And when they go there, maybe 10 children have been born, and they have not been vaccinated. The data will show that all of them have zero doses. So, that is the gap that we have.
Secondly, there is insecurity. You can see now that some of the healthcare workers will not want to go out of the urban areas. They will stay in an urban health facility because of insecurity. You can see that most of our health facilities are being abandoned because of the bandits. Because the bandit will come there, kidnap you and start asking for ransom. But there’s a community residing there, and they have been missing a lot of opportunities for immunisation. And once a survey comes, the status of the security may have changed. And the surveyor can pick their settlements. So this is how Sokoto continues to show that a lot of people are not being reached. Because the survey cannot just pick Sokoto North, Sokoto South, where we have full access to everything. They can decide to go to Illela, in one village, where maybe for the last year, no healthcare worker has gone there. And that is how they will rank the state based on this outcome. These are the two major concerns.
Also, the last one we need to review, though, that one has been improved adequately, is the payment remuneration of our healthcare workers. It has improved; most of the promotion has been implemented. But we still have a high number of people whose salaries are very small and are not even enough to sustain them for a month. So some, they just switch to an additional business. So, by and large, I think these are the common concerns that still exist, and which vary from advocacy, social mobilisations, and other reviews of the manpower who can be able to overcome those issues with the state.